
Watch the YouTube version of this post:
In case you didn’t know, I’ve recently started posting video versions of my blog posts. Here’s the one for this post:
Please stay tuned for more videos in the future!
“We are what we eat.”
We all know this old saying is true, even if we don’t always act like it.
Our stomachs are the main point of entry for the macronutrients, vitamins, minerals, phytochemicals, etc. the body needs to keep it running in prime condition.
This is equally true for the brain which, after all, is an organ just like the heart, liver, and kidneys. It too needs a steady stream of nutrients for optimal function.
On the flip side, if we put garbage into the brain, garbage is all we should expect to get out. Poor nutrition – not surprisingly – leads to poor brain function: fuzzy thinking and fuzzy emotions.
Poor nutrition is perhaps the most overlooked contributing factor of poor mental function and poor emotional states.
Diet and Drugs should work together
We treat depression and anxiety mainly in two ways: 1) psychotherapy and 2) drugs.
I am not opposed to these treatments. In fact, let me kick off this series of blog posts with a warning: if you are currently taking medication for depression and anxiety, do not stop just because you change your diet.
Most antidepressants and benzodiazepines are designed to increase or enhance the effects of critical brain chemicals. Quitting them cold turkey can have dangerous biochemical consequences, so please follow your doctor’s advice on when and how to stop.
But what I am saying is this: the food we eat should work with the drugs, not against them.
Let’s say I have high cholesterol levels. My doctor sits me down and gives me a serious talking-to: if I don’t get my cholesterol under control, my clogged, inflamed arteries will eventually cause problems, maybe a heart attack or stroke. So she prescribes statin drugs to help bring my cholesterol levels back down to normal.
But then my doctor does something else: she tells me that I must also watch my diet. I can’t gorge on greasy burgers and fries and cheesecake anymore.
I may not like the new rules, but I have to admit they makes sense.
I can’t just load up on all the cholesterol I want and hope the drugs will just vacuum it all back out.
Likewise, I can’t load my brain cells with garbage and hope that the antidepressants or benzos I’m taking will work some sort of magic.
As they say: garbage in, garbage out.
Diet and drugs should work together, not at cross purposes.
Now, of course the ultimate goal is that lifestyle changes (diet, exercise, rest, etc.) will make us all less dependent on drugs – maybe to the point where we won’t need them to keep us chugging happily along.
But until you and I reach that point, we should at least make sure that our lifestyle at least supports what the drugs are trying to do.
For this reason, I will spend the next several blog posts talking about the nuts and bolts of brain nutrition.
The Stress Cycle
If I were to ask you to describe your mood over the past several days/months, would the following come to mind?:
- Sprightly and upbeat (think Big Bird on Sesame Street)
- It’s easy to wake up in the morning and jump into the day
- Full of energy
- Enthusiastic about what’s going on in your life
- Relatively chill and relaxed; able to handle minor crises without an emotional meltdown
- Happy
- Content
- You savor the company of friends and loved ones
Or would you instead say something like:
- Cranky (Oscar the Grouch)
- It’s hard to drag out of bed on most days
- Full of fatigue
- Stressed out about what’s going on in your life
- On pins and needles; often over-anxious or angry over minor crises
- Sad or scared
- Irritable
- You are steering clear of friends and loved ones
The latter list can be symptomatic of one or more poor mental states: chronic stress, clinical depression & anxiety, and chronic fatigue. The three often go together, creating a Stress Cycle:

When we feel stressed out, we often try to self-medicate with highly processed foods loaded with plenty of salt, sugar, and fat.
There are even scientifically valid reasons why this happens.
Highly processed foods that come in takeout boxes or cardboard boxes are usually the most convenient, so they seem to fit better into stress-filled schedules.
“Comfort” foods like pizza, fries, pastry, and candy provide a quick shot of mood-altering chemicals that make us feel comforted and happy. Sugar-filled treats provide a quick source of energy, as does a cup of caffeinated whatever.
The problem starts when the sugar high wears off or the caffeine gives us a headache and brain drain. The brain takes a biochemical tumble, making us feel even more tired, stressed, and depressed than we were to begin with.*

This creates a vicious cycle:1
- We eat to feel better.
- The foods we eat (filled with sugar, salt, fat, and caffeine) provide only a temporary mood fix.
- We feel better at first, then we feel worse.
- We eat to feel better.

The Bottom Line
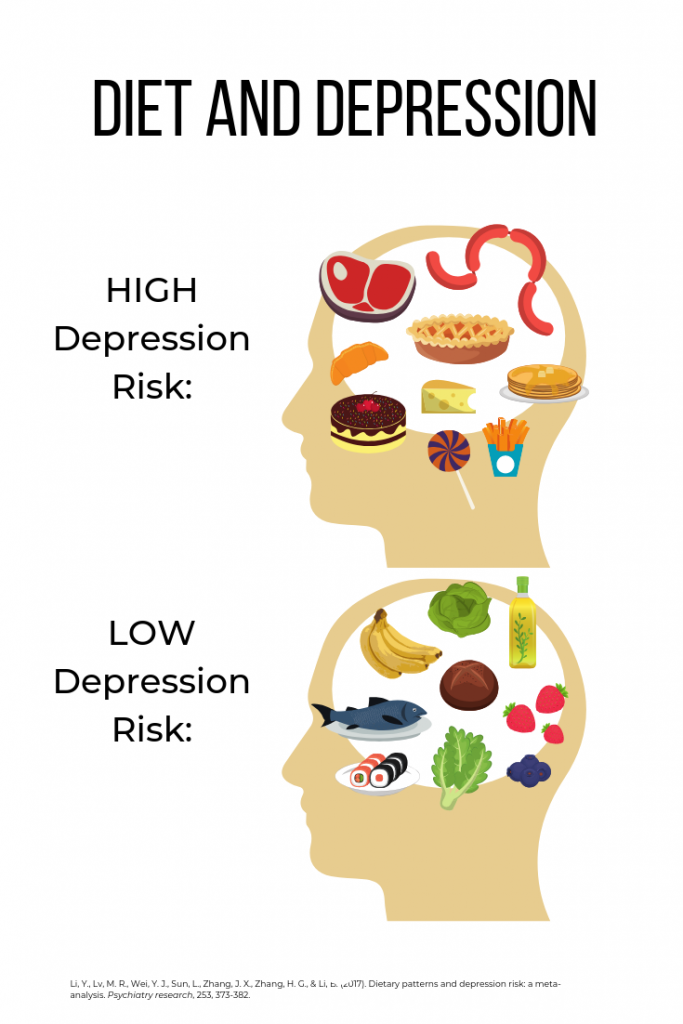
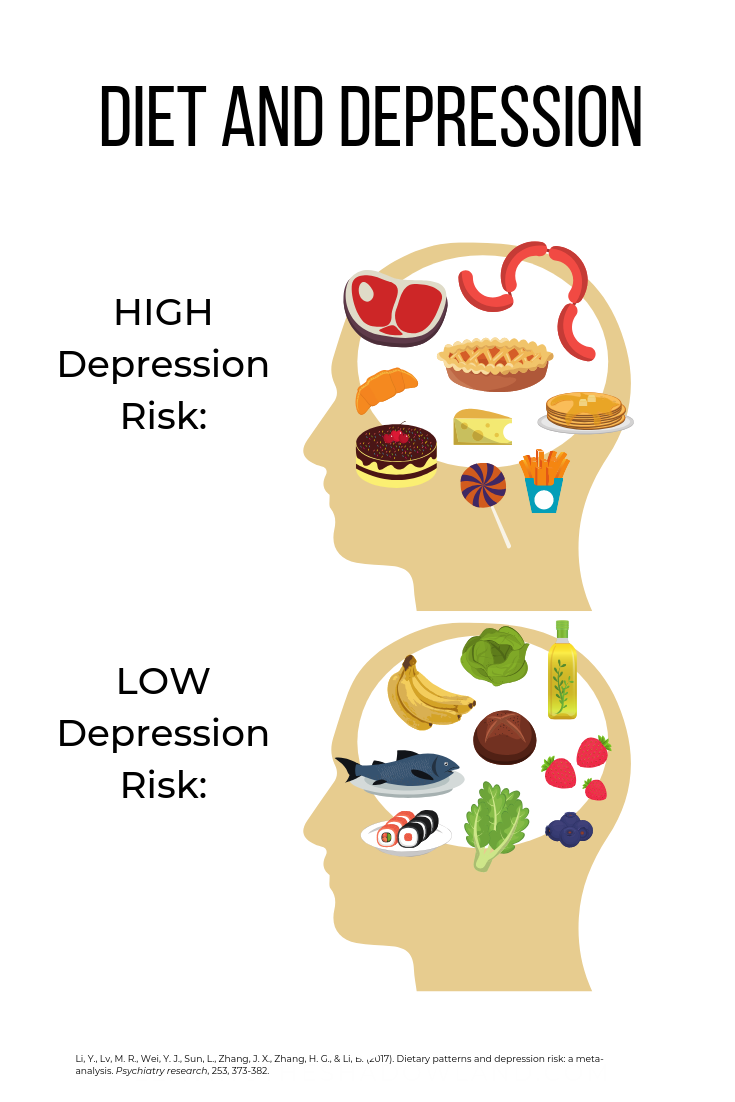
Large-scale studies involving hundreds of thousands of research participants have shown that eating a diet heavy in red meat, processed meat, refined grains, unhealthy fats (full-fat dairy products), and sugar increases the risk of developing depression.2
On the flip side, a healthy diet with plenty of fruits, vegetables, antioxidants, whole grains, low-fat dairy, soy, and healthy fats (olive oil and fish) has been shown to reduces depression risk.2*
I’ve seen a lot of press on the benefits of specific diets for mental health – the Mediterranean Diet, for example. However, a recent, large-scale research study showed no statistical difference between the Mediterranean Diet and others with the same characteristics: a (mostly) vegetarian diet or the Tuscan Diet.3
Over recent decades, the world’s dietary patterns have been going in the wrong direction: processed foods filled with refined sugars and unhealthy fats have replaced fiber, nutrient-dense foods, and healthy fats.4
The bottom line seems pretty clear: for optimal mental health, we need to turn this diet trend around. We need to start filling up on plenty of high-quality produce and healthy fats while eschewing sugar, extra salt, unhealthy fats, and animal products.
Here are some other links you might find helpful:
https://www.spiritofchange.org/food-cooking/5-Juice-Recipes-For-Depression/
https://mentalhealthfood.net/category/mental-health-recipes/
https://www.myfooddata.com/articles/high-tryptophan-foods.php
https://www.dietandfitnesstoday.com/tryptophan.php
1 Massey, A., & Bean, A. (2006). Improve Your Mood With Food. Virgin Books. p.14
2 Li, Y., Lv, M. R., Wei, Y. J., Sun, L., Zhang, J. X., Zhang, H. G., & Li, B. (2017). Dietary patterns and depression risk: a meta-analysis. Psychiatry research, 253, 373-382. (Data from 21 studies involving 117,229 participants were included in the this meta-analysis.)
3 Molendijk, M., Molero, P., Sánchez-Pedreño, F. O., Van der Does, W., & Martínez-González, M. A. (2018). Diet quality and depression risk: a systematic review and dose-response meta-analysis of prospective studies. Journal of affective disorders, 226, 346-354.
4 Popkin, B. M. (2015). Nutrition transition and the global diabetes epidemic. Current diabetes reports, 15(9), 64. Drewnowski, A., & Popkin, B. M. (1997). The nutrition transition: new trends in the global diet. Nutrition reviews, 55(2), 31-43.
Dr. Pamela Coburn-Litvak has published research articles on exercise and stress in Neuroscience and Neurobiology of Learning and Behavior. Her latest book, Leaving the Shadowland of Stress, Anxiety, and Depression, was published in 2020.
After receiving a Ph.D. in Neurobiology and Behavior from the State University of New York at Stony Brook, she served as both Assistant Professor of Physiology & Pharmacology and Special Assistant to the Vice President for Research Affairs at Loma Linda University in Loma Linda, California. She then joined the Biology department at Andrews University and developed courses in human physiology as well as the neurobiology of mental illness. She also founded Rock @ Science LLC, a company that specializes in health and science education and web development. She co-developed the brain and body physiology segment of the Stress: Beyond Coping seminar with its creator, Dr. William “Skip” MacCarty, DMin.
Dr. Coburn-Litvak currently lives in California with her husband. Their two daughters are mostly grown and attending school elsewhere.
When she’s not studying or teaching about stress, she enjoys stress-relieving activities like puttering around the garden, taking nature walks with her family, knitting, cooking, and reading.


[…] latest blog/video series I’m doing, called Food and Mood, is all about learning just what kinds of foods those […]
[…] We talked about the first six last week and will cover the final six this week. Both of these posts are part of my summer series, Food and Mood. […]
[…] noticed, but these same foods have come up repeatedly over the past several weeks of this Food and Mood series. So, chances are you’ve been steadily increasing these foods, anyway. If so, good on […]
[…] it turns out, this is not the only deep connection between feelings and food. Part 8 of my series on Food and Mood tells the tale of the gut-brain […]
[…] we wind down this series of Food and Mood, I thought I’d run through a top ten list of foods you and I should be eating regularly for […]
[…] this series on Food and Mood, we have taken an in-depth look at the specific nutrients needed for optimum mental and emotional […]