
By definition, action takers do not take stressful situations lying down.

But what kinds of action steps are the best to take?
The American Heart Association has outlined several physical and mental action steps we can take to address the stresses of life:
1. Relax.
Huh?
The first thing on our list is to start doing more…of nothing?
Well, yes. And the reason is, many physical stressors (accidents, illness, etc.) result from poor sleep and poor concentration.
Poor sleep is linked to greater risk of high blood pressure, diabetes and metabolic syndrome1 as well as depression.2 In a recent study of firefighter paramedics, sleep was found to impact their ability to deal with traumatic events. More specifically, sleep was one of the factors that determined whether they remained resilient or conversely developed symptoms of Post-Traumatic Stress Disorder (PTSD).3
So one way to avoid at least some types of physical or emotional stress is to relax more and get better quality rest.
Easier said than done, right?
Some of us are wound up so tight that relaxation seems an impossible pipe dream.
Try a few of these tips:
- Integrate relaxation into your day through progressive muscle relaxation and deep breathing techniques.
- Get exposed to bright, outdoor light for at least 30 to 60 minutes per day.
- Limit your exposure to blue-light emitting devices (laptops, smartphones, etc.) for at least 2 hours before bedtime.
- Take a walk every day. But don’t exercise too close to bedtime, which revs up the body and makes it harder to relax.
- Start a bedtime ritual that includes winding down work projects and turning off media devices. This puts your brain into “Now it’s time to rest” mode.
- Try this nightly relaxation technique by the National Sleep Foundation
2. Spend at least 15 minutes a day doing something that brings you joy.
The first obvious benefit: this will help relax you. But joy-filled projects or hobbies also provide a much needed mental vacation, a little oasis to look forward to in an otherwise hectic day.
Joy-filled, recreational activities also help reduce feelings of distress. In clinical populations, recreational therapy has been shown to successfully reduce symptoms of depression.4
In the general population, those who participate in recreational arts (e.g. painting, singing, dancing)5 or spend time in green spaces6 report having better mental well-being than those who don’t.
So go ahead – take a walk or bike ride through the local park, join a community club, indulge in your favorite hobby.
You are doing your brain some good.
3. Add one healthy habit this week.
Here are a few suggestions:
- Drink a little more water every day. Here’s a short, science nerd explanation for why this is important: dehydration causes our blood plasma to become more concentrated. To correct this, water is leached from nearby cells in the body and returned to the bloodstream.
When this happens in the brain, it can change brain structure and function.7
In contrast, better hydration combats feelings of fatigue, sadness, depression and anxiety; calms the nerves, and improves mental function.8
- Eat a little more fruit and vegetables. A large study of almost 300,000 people recently confirmed what we kind of already suspected: the more fruit and vegetables you and I eat, the less risk we have for depression.9
There is an equally nerdy explanation for why this is, but I will wait for a couple weeks to disclose it. This is because nutrition is such an important action step that it deserves at least one blog post of its own – maybe two or three.
Here’s the short version: fruit and vegetables have high payloads of vitamins, minerals, and other substances used in the production of several important brain chemicals. These brain chemicals affect our mood and motivational state.
So, there you go: more fruit and vegetables: more vitamins and minerals: more brain chemicals: better mood.
But there was something in particular that struck me about this study: even a little more can make a difference. An average serving of vegetables is 75 grams; a serving of fruit is 100 grams. The researchers reported that every 100 g of fruit or vegetables consumed decreases depression risk by a small percentage.
My take-home point is this: just one more serving a day will do your brain some good.
- Exercise more. Exercise has been used as a treatment for depression for a long time now and can be as effective as taking antidepressants.10
The medical journal Lancet recently published a study on the mental benefits of exercise in 1.2 million Americans.11 Individuals who exercised more (but otherwise matched non-exercisers in terms of sociodemographics and physical characteristics like Body Mass Index) had more than 40% fewer days of poor mental health in a month.
4. Use more stress-reducing beliefs.
I recently blogged about three of the most powerful stress-reducing beliefs I know of:
- Follow the Serenity Prayer: “Lord, give me the serenity to accept the things I cannot change, the courage to change the things I can, and the wisdom to know the difference;”
- Live One Day at a Time; and
- Believe there is Meaning in everything that happens.
I will cover more stress-reducing beliefs in future posts.
5. Engage in Positive Self-Talk.
While we often respond to stress in a physical way, really the more important actions happen in the mind.
Instead of getting lost in a mire of malignantly negative thoughts, we should, as quickly as possible, think of a positive path forward.
I discussed positive self-talk at length in my Cognitive Behavioral Therapy 101 series. When something bad happens, it is natural to ask ourselves why. To put thinking patterns in very general terms, we can either think:
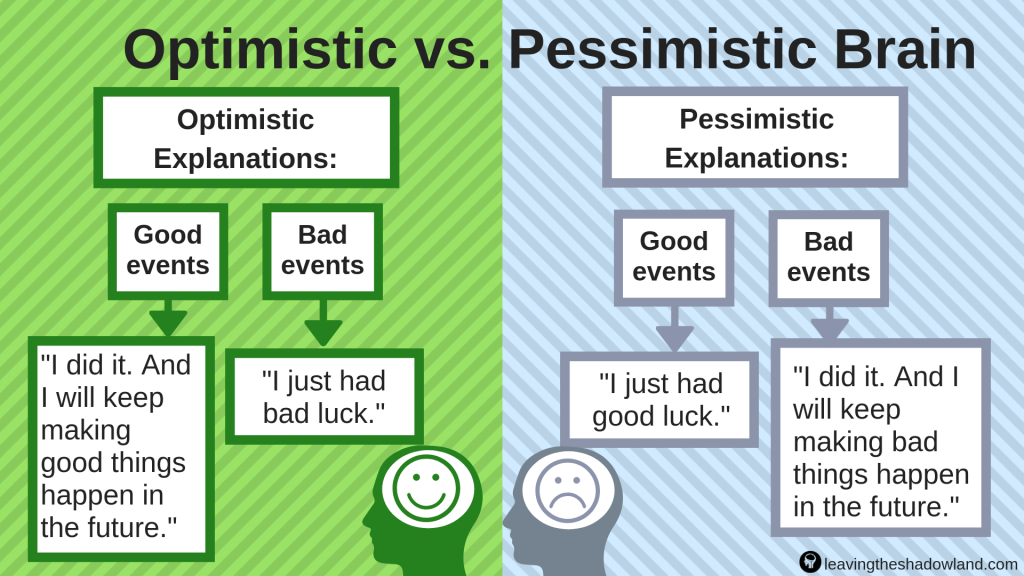
- Like a pessimist, which means blaming ourselves and believing that bad things will continue to happen in the future. As an example, let’s say that you text your best friend but don’t receive a reply. The pessimist would say, “Gee, I must have done something terrible to tick him or her off. I’m such a loser. We probably won’t ever be friends again.”
- Like an optimist, which means we find a reasonable explanation that is external to ourselves. If an optimist does not receive a reply to his or her text, he or she will say, “Gee, I wonder what’s wrong with my friend. What can I do to help?”
There’s a lot we could unpack here, but in a nutshell, positive self-talk involves:
- jumping to a positive conclusion first, not last;
- believing the best in others;
- believing the best in oneself;
- trusting that difficult situations are fixable and that they won’t last forever.
If you are interested in learning more, I would highly recommend books by Dr. Martin Seligman, a professor of psychology at the University of Pennsylvania and a pioneer in the field of positive psychology.
I am currently reading two of his books: The Hope Circuit and Learned Optimism.
Looking Ahead
Exercise is such an important topic that I will re-visit it next week.
I’ve been interested in this topic for a long time – I started publishing research articles on the mental health benefits of exercise while I was still in graduate school.
Since then, researchers have learned even more about how exercise can treat or prevent mental illness. I will discuss their findings – and give you a specific prescription for exercising for the best mental health – in next week’s post.
1 Brindle, R. C., Buysse, D. J., & Hall, M. H. (2018). Poor Cardiometabolic Health Is Related To An Aggregate Measure Of Sleep Health In A Nationally Representative Sample Of Americans: Results From The Midlife In The United States (MIDUS) Study. Sleep, 41(suppl_1), A331-A331.
2 Sun, Y., Shi, L., Bao, Y., Sun, Y., Shi, J., & Lu, L. (2018). The bidirectional relationship between sleep duration and depression in community-dwelling middle-aged and elderly individuals: Evidence from a longitudinal study. Sleep medicine.
3 Straud, C., Henderson, S. N., Vega, L., Black, R., & Van Hasselt, V. (2018). Resiliency and posttraumatic stress symptoms in firefighter paramedics: The mediating role of depression, anxiety, and sleep. Traumatology, 24(2), 140.
4 Flint, S. W., Lam, M. H. S., Chow, B., Lee, K. Y., Li, W. H. C., Ho, E., … & Yung, N. K. F. (2017). A systematic review of recreation therapy for depression in older adults. Journal of Psychology and Psychotherapy, 7(2).
5 Davies, C., Knuiman, M., & Rosenberg, M. (2015). The art of being mentally healthy: a study to quantify the relationship between recreational arts engagement and mental well-being in the general population. BMC public health, 16(1), 15.
6 Wood, L., Hooper, P., Foster, S., & Bull, F. (2017). Public green spaces and positive mental health–investigating the relationship between access, quantity and types of parks and mental wellbeing. Health & place, 48, 63-71.
7 Wittbrodt, M. T., & Millard-Stafford, M. (2018). Dehydration Impairs Cognitive Performance: A Meta-analysis. Medicine and science in sports and exercise, 50(11), 2360-2368.
8 Benton, D., & Young, H. A. (2015). Do small differences in hydration status affect mood and mental performance?. Nutrition reviews, 73(suppl_2), 83-96.
9 Saghafian, F., Malmir, H., Saneei, P., Milajerdi, A., Larijani, B., & Esmaillzadeh, A. (2018). Fruit and vegetable consumption and risk of depression: accumulative evidence from an updated systematic review and meta-analysis of epidemiological studies. British Journal of Nutrition, 119(10), 1087-1101.
10 Kvam, S., Kleppe, C. L., Nordhus, I. H., & Hovland, A. (2016). Exercise as a treatment for depression: a meta-analysis. Journal of affective disorders, 202, 67-86.
11 Chekroud, S. R., Gueorguieva, R., Zheutlin, A. B., Paulus, M., Krumholz, H. M., Krystal, J. H., & Chekroud, A. M. (2018). Association between physical exercise and mental health in 1· 2 million individuals in the USA between 2011 and 2015: a cross-sectional study. The Lancet Psychiatry, 5(9), 739-746.
Dr. Pamela Coburn-Litvak has published research articles on exercise and stress in Neuroscience and Neurobiology of Learning and Behavior. Her latest book, Leaving the Shadowland of Stress, Anxiety, and Depression, was published in 2020.
After receiving a Ph.D. in Neurobiology and Behavior from the State University of New York at Stony Brook, she served as both Assistant Professor of Physiology & Pharmacology and Special Assistant to the Vice President for Research Affairs at Loma Linda University in Loma Linda, California. She then joined the Biology department at Andrews University and developed courses in human physiology as well as the neurobiology of mental illness. She also founded Rock @ Science LLC, a company that specializes in health and science education and web development. She co-developed the brain and body physiology segment of the Stress: Beyond Coping seminar with its creator, Dr. William “Skip” MacCarty, DMin.
Dr. Coburn-Litvak currently lives in California with her husband. Their two daughters are mostly grown and attending school elsewhere.
When she’s not studying or teaching about stress, she enjoys stress-relieving activities like puttering around the garden, taking nature walks with her family, knitting, cooking, and reading.



[…] This post also appeared on another website of mine, Leaving the Shadowland. It was originally posted on January 23, 2019. […]